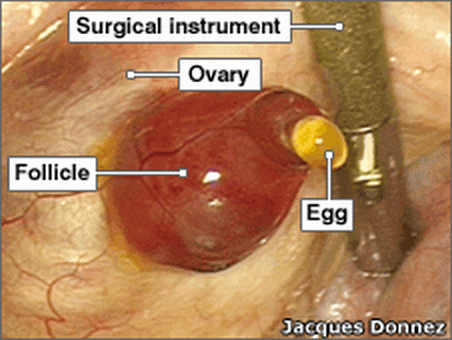
WHY FOLLICULOGENESIS IN VIVO™
In a nutshell:
Uniquely accurate fertility tracking. Detects ovulation. Records women’s 5th vital sign profile signatures for physicians.
Expanding somewhat:
Our ovulographic™ cervix-monitoring of folliculogenesis in vivo captures the fine-tuning neurological effects on folliculogenesis that are due to the direct neural control via ovarian and uterine innervation.
.
Right-click on the image for better legibility & two clickable links.
.
Why do this? Because, even though some women would claim they know when ovulating and their doctors would believe they have regular menstrual cycles, it has been known for decades that “…regularity was not demonstrated in as few as six cycles… When the number of cycles was extended to 12, no woman had variability of less than two days in cycle length” (See Major studies… for reference -right-click to open in a new tab).
In this day and age, many women reach for one of the ovulation predicting products that are in great demand, to try assessing their fertility status for fertility awareness. You or your “significant better” may be one of them.
The Folliculogenesis In Vivo™-monitoring personal home-use smart sensor, the Ovulona™, is unique and superior compared to the many existing commercial products in the category of home-use fertility self-help. That’s including the urinalysis LH hormone kits or OPKs (Ovulation Prediction Kits) and their improved electronic iteration. And including other products such as the currently popular smartphone apps based on the users’ BBT (Basal Body Temperature) aka the Waking Temperature.
The Ovulona is superior on several levels, for a number of reasons.
Unprecedented user-friendly design is made possible by the unprecedented accuracy of determination of ovulation and of the so-called fertile window, liberating the user from the consequences of the old imperfect-methods-based estimates of ovulation.
That must be the main advantage for the TTC (Trying-To-Conceive) people, but additional attributes are no less significant. Our technique’s broad applicability includes the inherent immediate detection of pregnancy and early pregnancy monitoring.
The latter is to help manage and deal with the naturally high prevalence of early embryonic mortality (EEM) a.k.a. early pregnancy loss (EPL), spontaneous abortion – the chief complication of human gestation. (See https://biozhena.wordpress.com/2010/01/10/about-the-added-bonus-of-folliculogenesis-monitoring-automatic-pregnancy-detection .)
When the TTC hurdle is successfully dealt with, the EEM is the next obstacle on the way to overcoming the sub-fertility issue. Think about this for a moment. The EEM is Mother Nature’s design to deal preventatively with problems, some of which likely lead to the TTC challenge (aka sub-fertility or even infertility) in the first place…

There is more to the superior attributes and applicability of the FIV technology [FIV = Folliculogenesis In Vivo]. Readily thought about is the non-invasive natural birth control.
The Ovulona is an electronic tool for 21st Century’s NFP and/or FAM – that is Natural Family Planning and Fertility Awareness Method. Both of which we envision under the umbrella of Scientific Family Planning™, SFP™ and/or SFA™, Scientific Fertility Assessment™.
Cervical health screen and treatment
Once you become aware of how Folliculogenesis In Vivo works, it will be less of a surprise to learn that the Ovulona tissue biosensor will also provide a built-in, hence eminently affordable and private, cervical health screen – prospectively screening not only for pre-cervical-cancer tissue aberration but also for other sexually transmitted pathologies – and offering a novel approach to the disease treatment.
Treatment (as opposed to diagnosis), you wonder what that is about? It’s about the vaginal tissues being the most efficient route for administering medications, and very logical for a topical treatment, wouldn’t you think? Logical and potentially pretty effective for public health, once the menstrual cycle monitoring tool has become widely used due to its affordability and mass-market acceptance. The Ovulona with a medication-administering attachment when needed. That’s another part of the vision.
There are numerous other applications that the male managers of investment coffers tend to view as women’s issues that are not their manly concern. Such as the management of PMS and its debilitating form the PMDD; such as proper evaluation of EDD and EDC (Expected – not Estimated – Date of Delivery, and of Confinement for birthing); such as hormone therapy in peri-menopause, and related matters. All these are big issues of public health, notwithstanding the sentiments of said managers of other people’s money.

Intuition – Gil Bruvel http://www.liveinternet.ru/tags/surrealism/page7.html
Now, back to the primary and initial use of the FIV-via-the-cervix-tracking Ovulona. An overview in three slides: https://biozhena.files.wordpress.com/2018/03/wealth-of-info-elucidation-silent-3-slides-animated-ed.pps. (With more in printable PDF available here.)
Only this FIV technology can
Only the Ovulona can determine the three days of the fertile window of opportunity to conceive, unperturbed by the talk out there (by the proponents of the mentioned imperfect ovulation measures) about six fertile days, which talk stems from a certain highly publicized but flawed study in 1995. A NEJM publication caused a sensation at the time by shortening the NFP’s prescribed period of abstinence from the previous much too long imposition to the less off-putting 6 days. See https://v.gd/fCJSGH and grasp this gist of the message: Only the Ovulona-recorded menstrual cyclic profile can tie conceptions to specific cycle days.
The detection of the 3 fertile days is possible because the Ovulona monitors the process of folliculogenesis, and does it by sensing the tissues in the reproductive tract where the site of action is. That’s where the female body integrates and responds to signals from the ovary and from the brain. The response is the action, as opposed to the mere presence of this or that hormone detected in blood or urine or any other body fluid.
The determination of the 3-day window is absolutely necessary because only that way can conception be either enabled or avoided with the required accuracy. The existing fertility tracking home-use products cannot do that, and that is why they speak about a longer and fuzzy fertile window.
See relevant posts in bioZhena’s Weblog if you want to get a better understanding of all that which is covered by the short word fuzzy. https://v.gd/9hCBKU is one relevant post. You will get to understand why “peri-ovulation methods” is the fitting descriptor of the prior art methods in https://v.gd/az4Xys.
Neither can the existing commercial products be used for an attempt at baby gender pre-selection by timing conception with respect to ovulation. They cannot do that because they do not anticipate ovulation accurately, and they do not detect ovulation – they merely guesstimate and assume its occurrence.

Toyen, Spící (1937) http://kultura.idnes.cz/podivejte-se-jak-vypada-marne-cekani-od-toyen-ktere-se-drazi-za-20-milionu-1ak-/vytvarneum.aspx?c=A090312_102133_vytvarneum_jaz The title means Sleeping. The referenced source media article’s title says : Look what futile waiting by Toyen looks like… Incidentally, Toyen was a rebel, even more so than Margaret Sanger – or rather, Sanger would next to her probably not qualify for the rebel label… See Description of the image file for more about Toyen: https://biozhena.wordpress.com/2012/05/14/why-too-many-young-and-not-so-young-ladies-could-not-receive-flowers-on-mothers-day-why-so-many-trying-to-conceive-why-so-much-infertility/toyen-spici-1937/ It is not likely that Toyen would have had this in mind, but I present her art to highlight the predicament of unfulfilled yearning for a baby. To highlight this: The probability of becoming pregnant is critically dependent on whether the insemination (natural or artificial) occurs at the right time, within the fertile window. This is because the probability of pregnancy is a combination of four individual probabilities: 1. Probability of being in good health, 2. of successful insemination, 3. of not miscarrying the conceptus, and 4. the probability of correct timing of the conceptive intercourse. For example, a 60% success rate of correct timing brings the overall probability of pregnancy down to a mere 36%, and this goes down to a mere 30% if correct timing probability is only 50%, in healthy fertile couples assuming the probability #3 (not miscarrying the conceptus) at an optimistic 75%. Even if the probability of determining the insemination time correctly were 90%, the resulting probability of successful pregnancy from any one particular insemination event would be only 55%. Get this! Only 55% under perfect ideal conditions, which include a young healthy unstressed woman.
Consequently, those technologies cannot pinpoint the 2 days before and the day of ovulation. This detection of the 3 days is needed for trying to conceive a boy or for trying to conceive a girl, when trying to get pregnant. For more see https://v.gd/3xndsX.
Your Fertility Awareness tool for natural birth control
And the ability is needed for avoiding conception, i.e. for avoiding pregnancy. The commercially available ovulation estimating technologies do not detect ovulation independently of the one predictive hormone that they test for – or two such hormones, LH and E2, in the case of the urine-analyzing gadget sold by the mighty P&G in joint venture with SPD GmbH. But for the user relying on that is not unlike groping in the dark…
Of the other electronic gadgets out there, the one offered by Zetek, is tracking indirectly the effect of the same hormone (estrogen, E2) in two body fluids with two probes at two different times during the menstrual cycle.
And then there is your old BBT method – implemented by several costly products and utilized by many smartphone apps. The BBT tracks indirectly the effect of progesterone that you know causes the BBT to go up a bit after ovulation, albeit with a statistical uncertainty of + or – 3 days, and a poor signal to noise ratio and interference from responding to non-related things at that. (See single narrated slide overview of competition at https://v.gd/b696FF.)
All those old *Imperfect Measures* tools detect a hormone input (or two) within the hormone signaling mechanism. However, the boundaries of the fertile window are not single hormone events. Circulating hormone monitoring – direct or indirect – cannot define the fertile window. The existing ovulation prediction products do not determine the fertile window of 3 days because they monitor this or that remote parameter that only reflects some pre-ovulation aspect of folliculogenesis, the process that culminates in ovulation.
The *Imperfect Measures* products only detect one of the hormone signals that says “ovulation can happen about now” (LH), or a signal that says “ovulation has occurred” (BBT); or some reflect estrogen (e.g., through the appearance of saliva).
Estrogen elevates before LH but not far enough ahead, and certainly it does not indicate the beginning of the true fertile window nor the end of the window (ovulation). The saliva property is a fuzzy indicator of estrogen, and similarly the vaginal fluid’s tactile and visual properties tracked by some NFP users. But accurate undistorted *perfect measure* of fertility must monitor the brain-ovary feedback.
See (right-click to open in new tab): https://biozhena.files.wordpress.com/2019/08/hpg-feedback-loop-w.-wakeup-calls-e1.pdf

Clock Explosion by Salvador Dali
.
Timing of ovulation varies, ovulation must be actually detected
Significantly, the hormones in circulation that anticipate ovulation do not mean that ovulation occurs as estimated or even at all. The hormones merely signal that the reproductive system is ready. The hormones do not show and do not tell whether or not the neurological part is a go, too. The cervix monitors the brain – ovary hormone feedback interactions, and we monitor the cervix. As one of the patents states, “an intelligent probe monitors folliculogenesis and correlates the ovarian function data to probe profile characteristics of the female reproductive cycle. A fertile window is defined with reference to the correlation between folliculogenesis and probe cyclic profiles.”
It is essential to detect the actual occurrence of ovulation independently of its prediction by the hormones. Only our technology does that. Only our technology anticipates ovulation quantitatively in daily reference to the menstrual cycle FIV profile, and then detects ovulation separately from the predictive data.
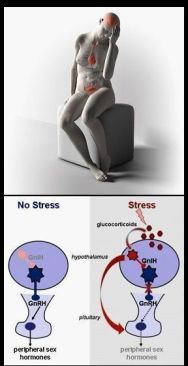
Stress often delays or even prevents ovulation – a surprisingly frequent occurrence (https://v.gd/QLjHD6). Only the Ovulona™ detects and works with this: https://v.gd/1jCnuO and https://v.gd/z4xCIJ. Only this FIV™ technology can.
There are bioZhena’s Weblog posts about the variability of ovulation timing from cycle to cycle in the same woman as well as across a population. The variability can be more than the width of the fertile window, more than the said 3 days dictated by the biology (the functional lifespans of the egg and sperm). The 3 day span tends to also be the statistical uncertainty of some of the old techniques, plus or minus 3 days. This is serious because for a woman’s sexual intercourse outcome every day matters, every day makes a difference.
Serious consequences ensue for the users of the old *Imperfect Measures* techniques, whether employed to achieve pregnancy or to avoid it. Look at the following example from a test-of-prototype study by an independent NFP [Natural Family Planning] research-and-teaching group.
 click to enlarge
click to enlarge
In the four recorded cycles of a childless 41-years old patient, the Ovulona prototype captured 3 delayed ovulations out of the 4 recorded cycles. In only one of the four cycles did the LH agreed with our ovulation marker while Peak Mucus indication was one day late in that cycle.
In her three cycles with delayed ovulation, the delays were:
In cycle 1, 4 days after LH kit positive and 3 days after Peak Mucus.
In cycle 3, 3 days after LH kit positive and 2 days after Peak Mucus.
In cycle 4, 1 day after LH kit positive and 2 days after Peak Mucus.
In an earlier post in this blog, I showed how the test data divides the NFP clinic patients’ results into two categories that we termed regular and irregular (challenged). To avoid confusion with the traditional usage of the terms regular and irregular in the context of menstrual cycles, we shall refer to the two categories as normal and challenged, respectively. Cycle 2 above is a normal cycle with LH and Peak mucus within 1 day of ovulation marker day versus the other records showing challenged cycles with delayed ovulation. (See blog post at https://v.gd/Va6GMQ.)
The other challenged cycles from the study are tabulated below here, and you will note that they are quite numerous even in the small study of just 10 women with 2 cycle records each. Even in that small population of real-life (non-baseline) women, 45% cycles were challenged. You also see that the ovulation delays occur at any age (here from 19 to 41 years of age), and regardless of parity (that is, regardless of whether the woman has ever borne children or not):
 click to enlarge
click to enlarge
In the table of ovulation days indicated by the three techniques, O stands for the ovulation marker of Ovulona prototype, LH means LH kit (OPK) positive result, and Pk means positive Peak Mucus result (as taught by NFP teachers).
As noted above, LH and Pk days are in all these cycles lower than the O days, which relationship defines the category of challenged cycles (ovulation delayed with respect to given hormone signal). The delays in this small sample from a small pilot study are from 2 days to 4 days with respect to LH, and from 2 to 3 days with respect to Pk; two cycles are without any LH surge detection.
And here now follows (again, if you did not miss it earlier) a hint at what the Ovulona will do for you, how it can work with the various challenged cycles. Take your time to take it in…
Look at these two successive cycle records that are suggestive of two ways of brain-ovary synchronization, the precondition of ovulation. In cycle 4, we see 2 days of ovulation delay after the short-term predictor peak; in cycle 5, we see 2 days of signal arrests on the descending branch of the dominant follicle maturation peak (the long-term predictor peak), with no ovulation delay after the short-predictor peak.
 Click on the image for better legibility in the captured PPS slide https://biozhena.files.wordpress.com/2020/09/single-slide-non-baseline-cycle-w-delayed-ovulation-algor-applied-and-next-cycle-no-ovu-delay-e2-arrests-stars.pps
Click on the image for better legibility in the captured PPS slide https://biozhena.files.wordpress.com/2020/09/single-slide-non-baseline-cycle-w-delayed-ovulation-algor-applied-and-next-cycle-no-ovu-delay-e2-arrests-stars.pps
Let’s also note that the Ovulona monitoring process – while generating the detailed folliculogenesis profile data essential for optional analysis by the woman’s healthcare provider – is not unpleasant as is urine sampling, and is not cumbersome, confusing or prone to subjective misinterpretation of results as the other techniques tend to be.
The Smart Ovulona™ will display for the user daily the interpreted result such as either NOT FERTILE or, as detected, FERTILE DAY 1, FERTILE DAY 2, or FERTILE DAY 3 = OVULATION. When appropriate, the display will also indicate PREGNANCY! or SEE DOCTOR ABOUT CERVIX (the latter when a cervical tissue aberration will be detected in several consecutive cycles – to avoid and liberate women from the known anxiety-causing problems of the Pap smear test).
We can and we do envisage the Ovulona use (and later the telemetric HaloTM cervical ring use) to become a friendly routine for the women of the 21st century, everywhere. The existing home-use fertility monitoring products could not aspire to play that role. Hormone detection in body fluids is only of temporary utility for the Trying To Conceive (TTC) women.
Folliculogenesis In Vivo is not only a superior tool for TTC but it goes beyond that first use – to be of unprecedented and unique service in personalized women’s healthcare for years to come. View 3 slides (Ovulona from startup version to cervical ring implementation): https://v.gd/paNdRr.
And see how the bioZhena technology will help physicians to better help their female patients (explore the links): https://biozhena.files.wordpress.com/2019/01/Single-slide-How-the-Ovulona-will-help-physicians.pdf.
You can find other relevant posts in bioZhena’s Weblog (here is clickable table of contents with snippets) and related articles about how symptoms (such as PMS symptoms) vary depending on the phase of the menstrual cycle and on the health conditions of any woman. It is known that female patients respond to therapy differently in relation to their menstrual cycle, i.e., in relation to folliculogenesis. That relationship between symptoms and the FIV profile is THE fundamental guiding principle of personalized medicine for women.
A new era of gynecology and obstetrics in the offing.

Folliculogenesis in vivoTM for women’s healthcare – the vision (from Space perspective, courtesy of NASA)
Yes, dear reader, contingent upon securing capital, both financial and human… ![]()